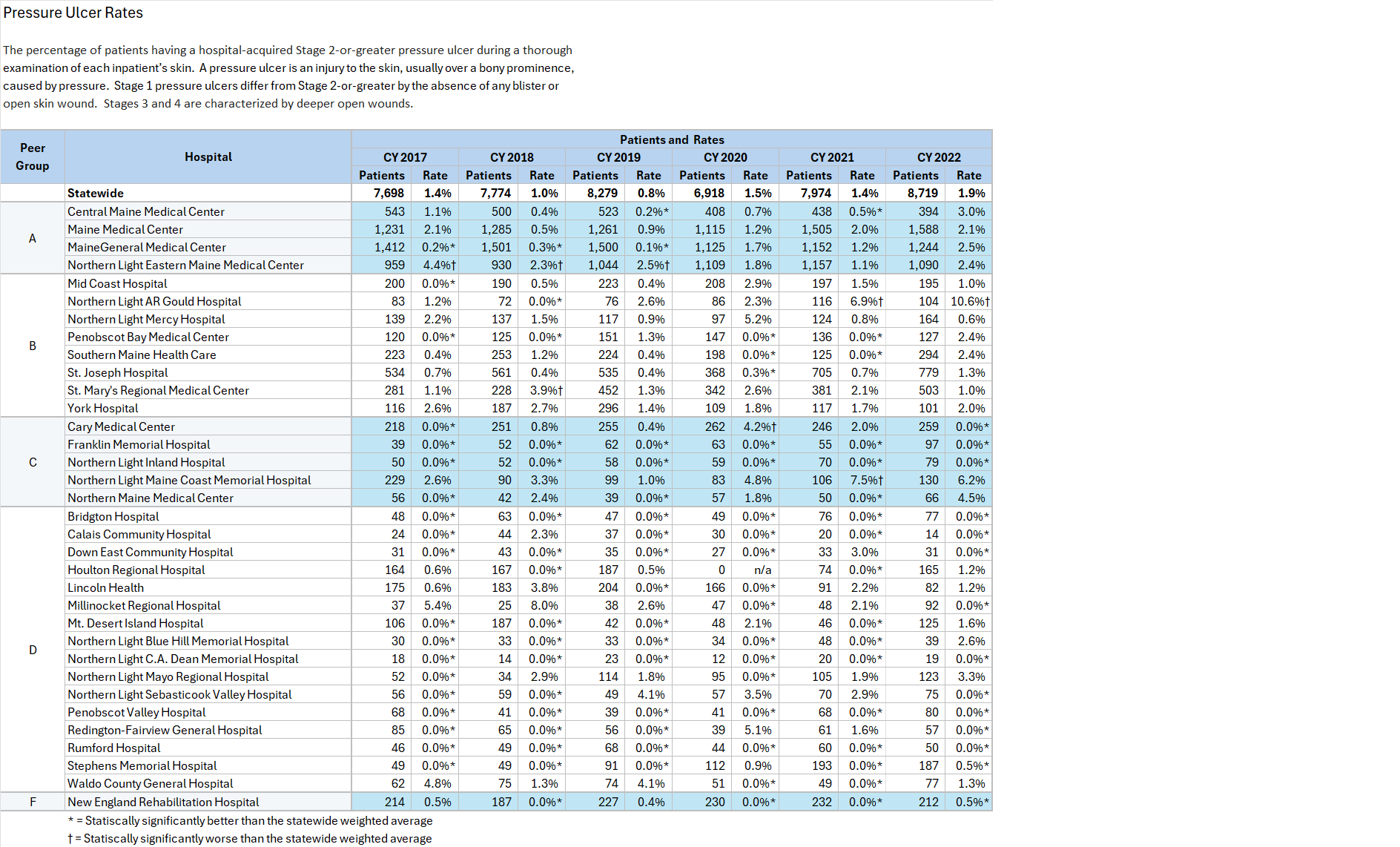
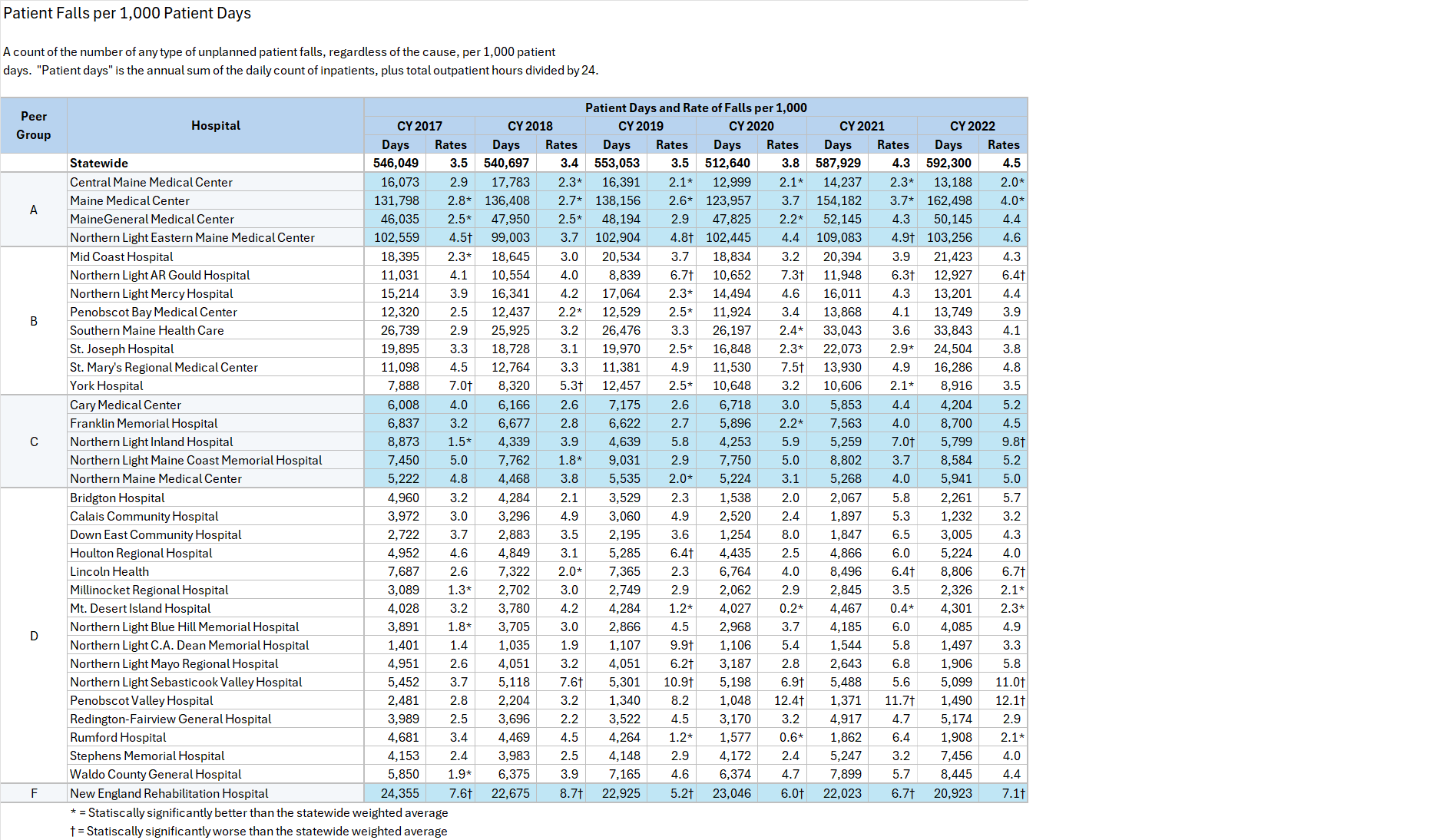
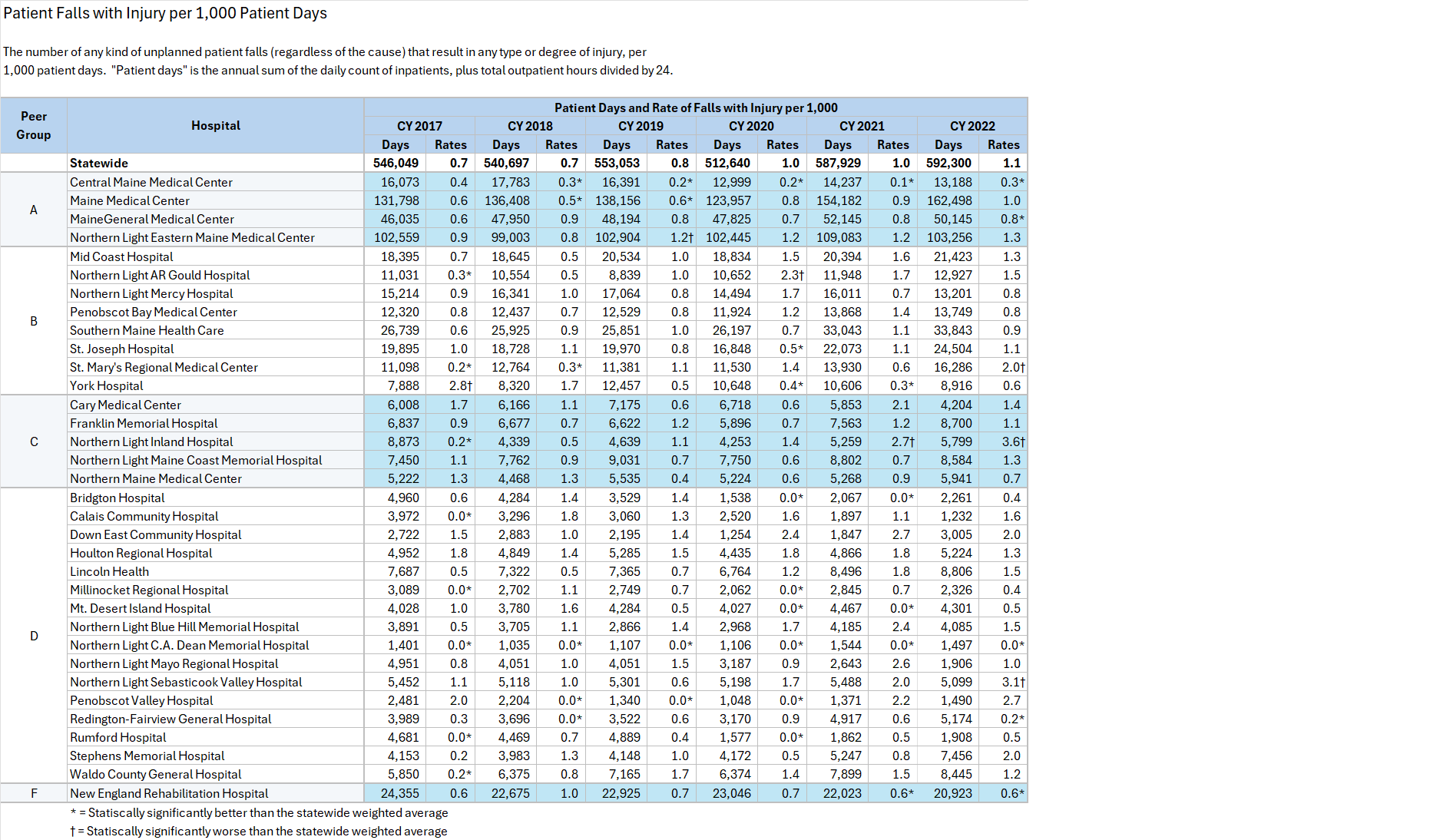
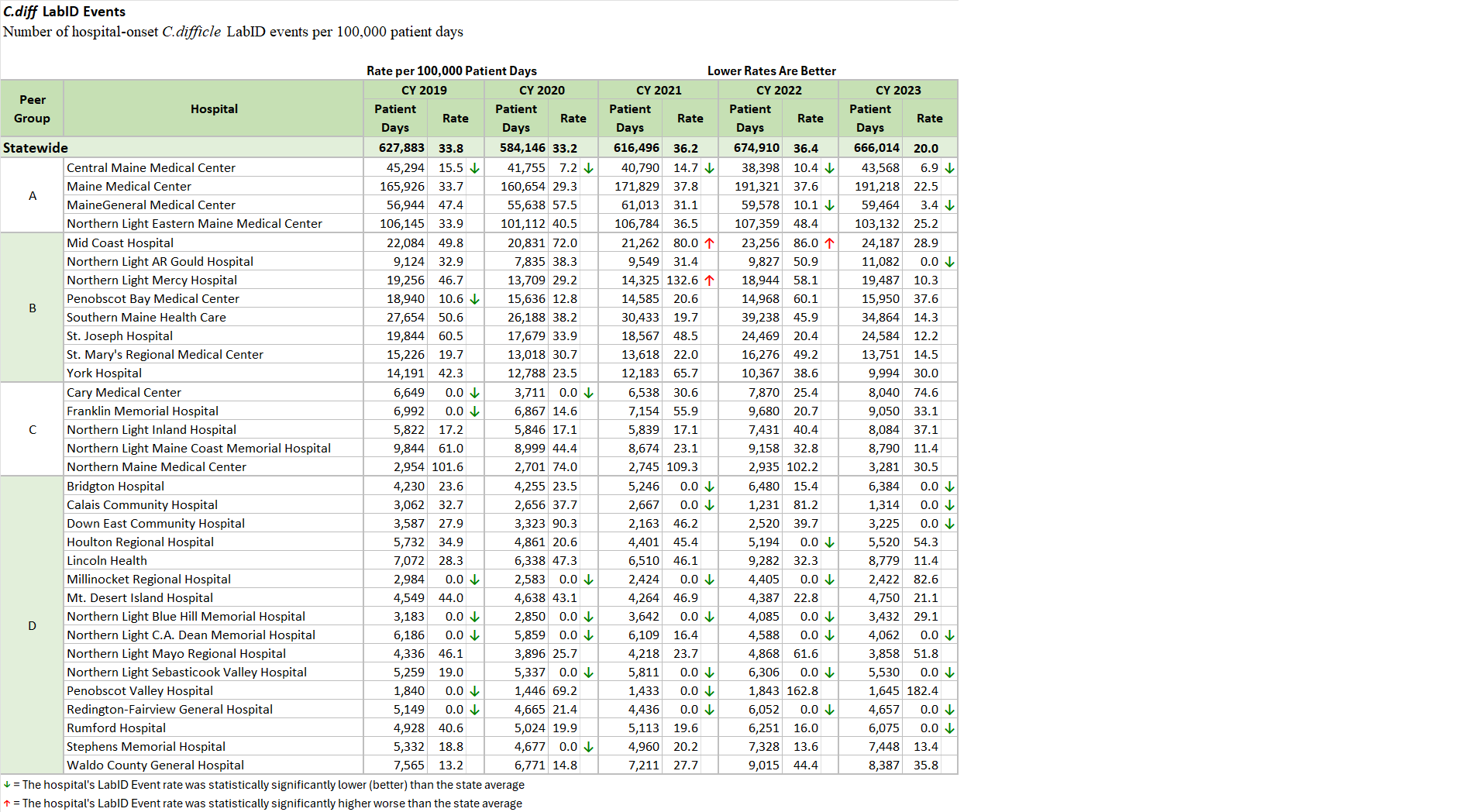
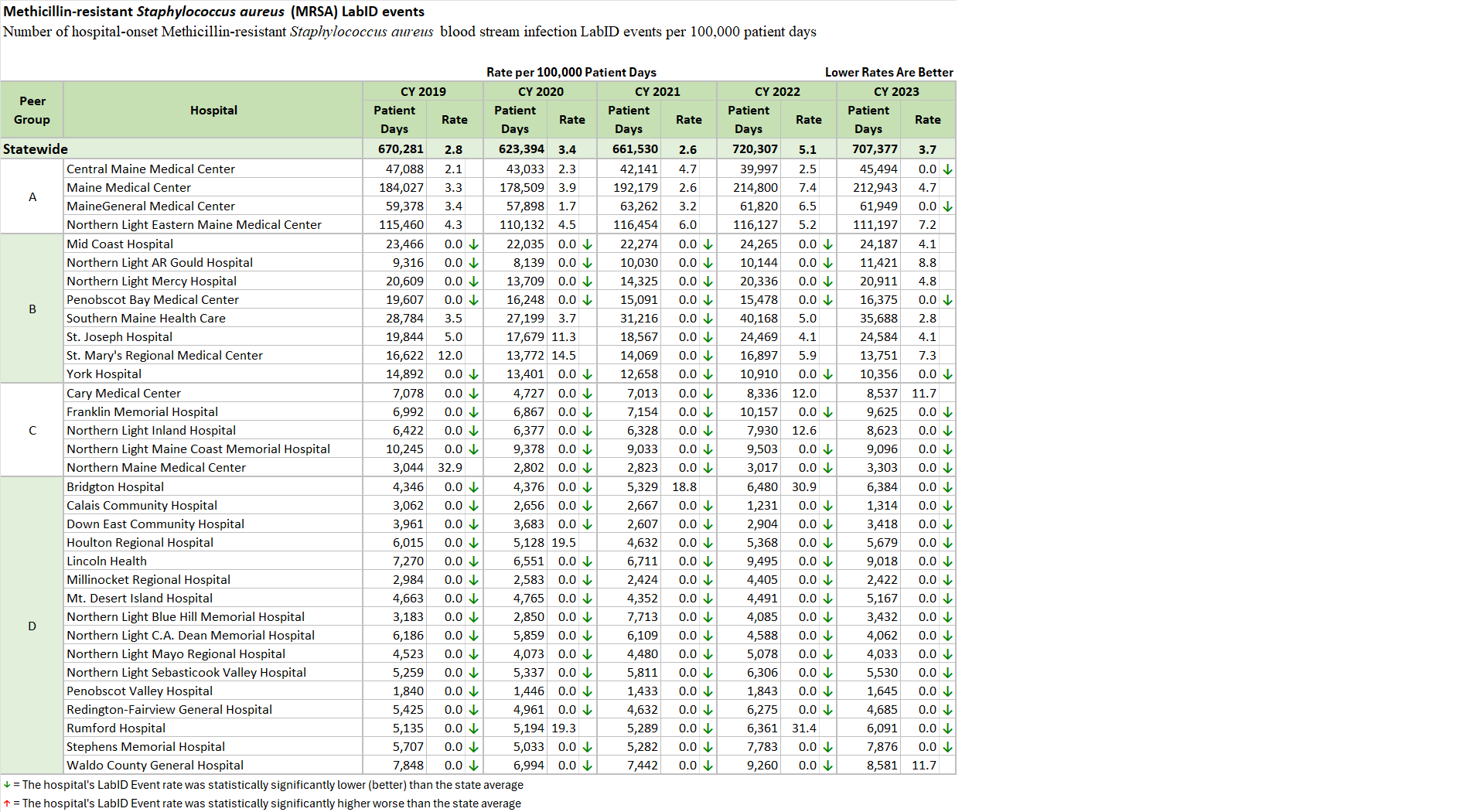
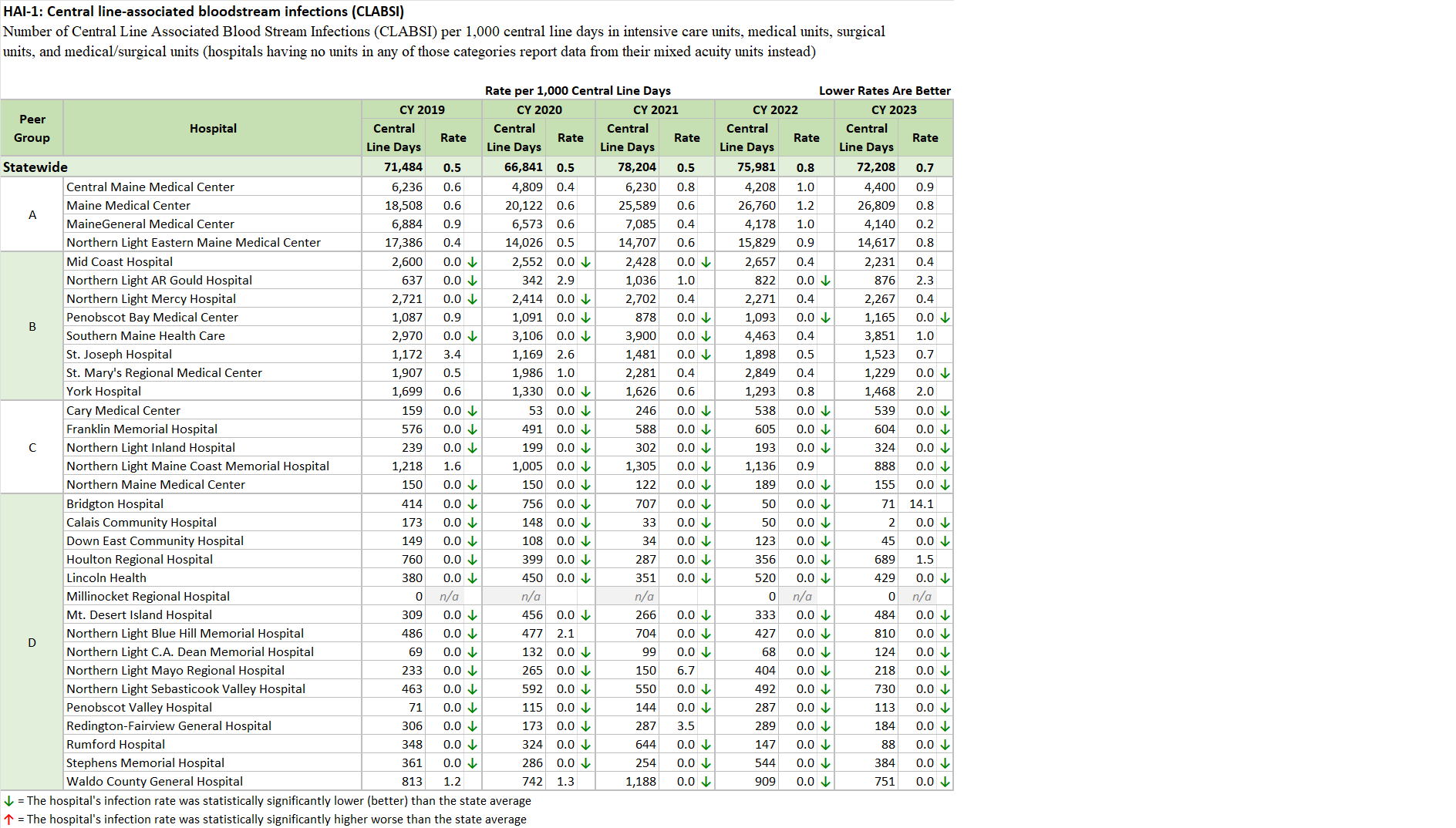
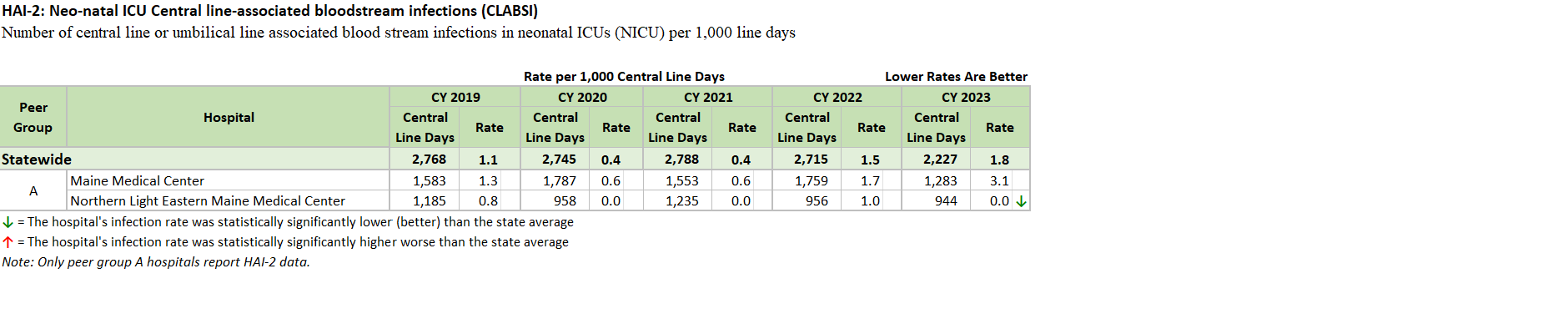
Maine Hospitals report quality metrics to the Maine Health Data Organization (MHDO) for Healthcare Associated Infection (HAI) measures specified by MHDO Rule Chapter 270 - Uniform Reporting System for Health Care Quality Data Sets. The tables (below) are based on this data. They display how each Maine hospital performed on each measure during a specified 12-month period. Trend charts depict the change in statewide weighted average performance for each measure over the past five years.
The hospitals are categorized by Peer Groups (as provided by the Maine Hospital Association) to allow comparison between hospitals of similar size.
(Note: Maine's four psychiatric hospitals and Togus-the VA Hospital are exempt from Chapter 270 reporting requirements.)
Select this link to download the Excel version of the HAI reports (C.diff, MRSA, CLABSI HAI-1, and CLABSI HAI-2) below.
Select this link to download the Excel version of the NSI reports (Pressure Ulcers, Patient Falls, and Patient Falls with Injury) below.